Knowledge Centre
Cardiology : Non-Invasive Procedures
ECG
An electrocardiogram (ECG / EKG) is an electrical recording of the heart and is used in the investigation of heart disease. Also known as an EKG (from the German language) or an ECG, this is the oldest heart test that is still in routine use today.
The ECG is a method of recording the electrical activity of the heart. Each heartbeat is caused by a section of the heart generating an electrical signal which then conducts through specialized pathways to all parts of the heart. These electrical signals also get transmitted through the chest to the skin where they can be recorded.
An ECG is performed by placing 12 recording leads at certain specific locations on the body. They only record the heart's electrical activity. They do not produce any electricity of their own. The test does not hurt and has no known side effects. It does not require any preparation (except for possibly shaving chest hair to get a better recording). The recording itself takes only a few seconds. Including the setup time and the time to disconnect the leads, the whole procedure takes about 5 minutes.
Why 12 leads?
Looking at the heart with 12 leads is like looking at a sculpture, building or car from multiple angles. The more points of view you have, the more you learn about it.
By looking at the electrical patterns on an ECG, your doctor can determine:
- The nature of an erratic heartbeat. There are many different types of abnormal heart beats. Not all require treatment. In those that do, the ECG recording lets the doctor know which treatment is best.
- The presence of a heart attack. It can also be determined whether the heart attack is old or recent.
- The possibility that there are narrowed arteries in the heart which may lead to a heart attack in the future.
- Whether or not discomfort in the chest is being caused by the heart.
- Degeneration of the conduction system of the heart which can lead to dangerously slow heart beats. This condition is often treated with a pacemaker.
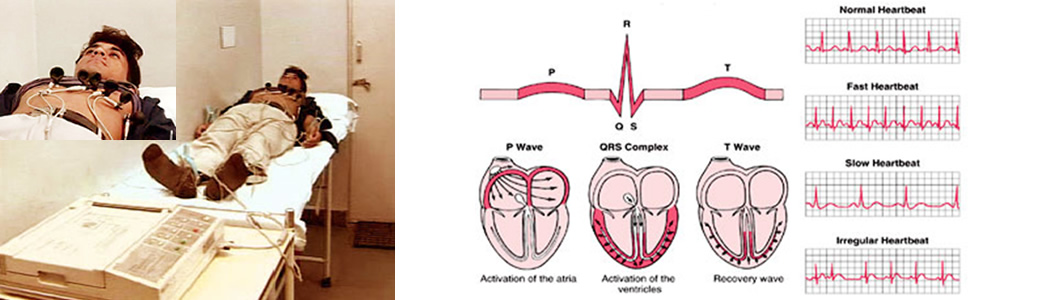
Tread Mill Test (TMT)?
Exercise is a common physiology stress used to elicit cardiovascular abnormalities not present at rest and to determine the adequacy of cardiac function. Tread Mill Test (TMT) is one of the most frequent non invasive modalities used to assess patients with suspected or proven CAD. The test is mainly used to estimate prognosis and to determine functional capacity, the likelihood and extent of CAD, and the effects of therapy. The treadmill protocol should be consistent with the patient's physical capacity and the purpose of the test. The Bruce multistage maximal treadmill protocol has 3-minute periods to allow achievement of a steady state before work-load is increased. In older individuals or those whose exercise capacity is limited by Cardiac Disease, the protocol can be modified by two 3-minute warm-up stages. The sensitivity of the Tread Mill Test (TMT) in patients with CAD is approximately 68%, and specificity is 77%. The exercise electrocardiography (ECG) result is more likely to be abnormal in patients with more severe coronary arterial obstruction, with more extensive CAD, and after more strenuous levels of exercise. The diagnostic accuracy of exercise-induced ST segment depression for obstructive CAD is less in women than in men. Exercise testing has an excellent safety record. The risk is greater when the test is performed soon after an acute ischemic event.
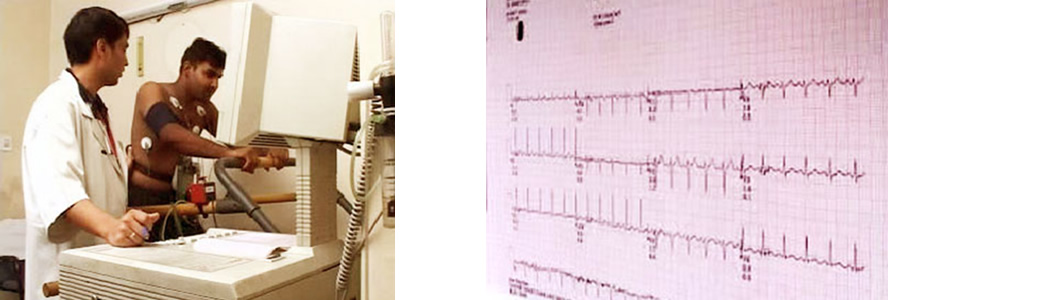
What is Echocardiography / Colour Doppler?
Echocardiography is the application of ultrasound for imaging of the heart. Standard ultrasound techniques are used to image two-dimensional slices of the heart. Apart from 2-D, conventional echocardiography also employs M-mode and Doppler is use to image flowing blood. Continues wave Doppler and Pulsed wave Doppler are used to measure the velocity of flowing blood. Latest developments in the field of echocardiography include real time 3-D imaging, tissue Doppler and many specialized techniques.
The usual echocardiogram is also known as a transthoracic echocardiogram, or TEE. In TEE, heart is imaged from outside through the chest wall. The echocardiography probe is placed on the chest wall of the subject and images are obtained. This is a simple, highly accurate test. Another method to perform an echocardiogram is to insert a specialized endoscope containing an echocardiography transducer in to the patient's esophagus and record pictures from there. This is known as a transesophageal echocardiogram or TEE. TEE has the advantage of giving better images. This is because the transducer is closer to the heart. Some of the posterior structures of the heart are better imaged with TEE. These include the aorta, the valve of the heart, and the left atrium. TEE requires light sedation and a local anaesthetic lubricant for the oesophagus and is slightly uncomfortable for the patients.
Holter
Holter monitoring provides a continuous recording of heart rhythm during normal activity. The monitor is usually worn for 24 hours to obtain a recording of a complete day. During a heart holter monitor study the electrical activity of the heart is recorded (similarly to the recording of an electrocardiogram), usually for a 24-hour period while a diary of the patient's activity is recorded during this period. The recording is then analyzed, a report of the heart's activity is tabulated, and irregular heart activity is correlated with activity.
TEE
A Transesophageal Echocardiogram (TEE) is a useful tool used to evaluate the function and small detailed structures of the heart and associated vessels. The Transesophageal Echocardiogram is a variation of the Transthoracic Echo procedure. The TEE procedure uses ultrasound waves to produce images of the heart. Performing a TEE involves passing a tube into the esophagus, or swallowing tube. In North America the test is performed and interpreted by a physician, usually a cardiologist, specially trained in Transesophageal Echocardiography.
If you are going to have a TEE it is more than likely that it has been requested or ordered by your physician or a cardiologist. There are many reasons for requesting that you undergo this procedure. Physicians use this procedure to look for any abnormalities in the physical structures of the heart, including the heart chambers, valves, and associated blood vessels. This procedure is sometimes also used to look for abnormalities within the structures that a standard transthoracic echocardiogram is not able to highlight. This may include examining the detailed structures and functioning of the heart valves.
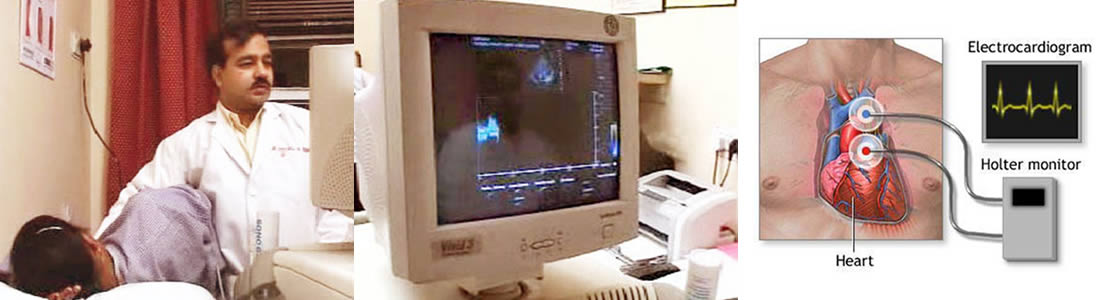
Cardiology : Interventional Procedures
Coronary / Renal / Peripheral Angiography
One way to unblock (open up the lumen) of a coronary artery (or other blood vessel) is percutaneous transluminal coronary angioplasty (PTCA), which was first performed in 1977. A wire is passed from the femoral artery in the leg (most commonly) or the radial artery in the arm up to the diseased coronary artery, to beyond the area of the coronary artery that is being worked upon. Over this wire, a balloon catheter is passed into the segment that is to be opened up. The end of the catheter contains a small folded balloon. When the balloon is hydraulically inflated, it compresses the atheromatous plaque and stretches the artery wall to expand. At the same time, if an expandable wire mesh tube (stent) was on the balloon, then the stent will be implanted (left behind) to support the new stretched open position of the artery from the inside.
Angioplasty and stenting is performed through a thin flexible catheter during Cardiac Catheterization with just a local anaesthetic to the groin (or wrist) where the catheter was inserted, often making heart surgery unnecessary. While coronary angioplasty has consistently been shown to reduce symptoms due to coronary artery disease and to reduce cardiac ischemia, it has not been shown in large trials to reduce mortality due to coronary artery disease, except in patients being treated for a heart attack acutely (also called primary angioplasty). There is a small but definite mortality benefit with this form of treatment compared with medical therapy, usually consisting of thrombolytic ("clot busting") medication.
Traditional ("bare metal") coronary stents provide a mechanical framework that holds the artery wall open, preventing stenosis, or narrowing, of arteries feeding critical structures like the myocardium. Traditional stenting is superior to angioplasty alone in keeping arteries open.
Newer drug-eluting stents (DES) are coated with drugs that prevent re-stenosis of the artery. Three drugs, sirolimus, everolimus and paclitaxel, have been demonstrated effective and safe in this application by stent device manufacturers and are being used.
Risks of angioplasty are fortunately uncommon, and the procedure is widely practiced. Coronary angioplasty is usually performed by an interventional cardiologist, a medical doctor with special training in the treatment of the heart using invasive catheter-based procedures.
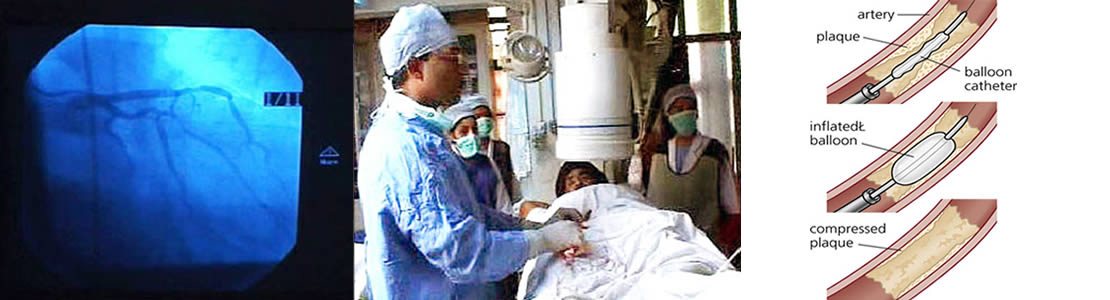
Cardiac Catheterization
This is a procedure done on the heart. In it, a doctor inserts a thin plastic tube (catheter) (KATH'eh-ter) into an artery or vein in the arm or leg. From there it can be advanced into the chambers of the heart or into the coronary arteries.
This test can measure blood pressure within the heart and how much oxygen is in the blood. It's also used to get information about the pumping ability of the heart muscle. Catheters are also used to inject dye into the coronary arteries. This is called coronary angiography (an"je-OG'rah-fe) or coronary arteriography (ar-te"re-OG'rah-fe). Catheters with a balloon on the tip are used in the procedure called percutaneous transluminal coronary angioplasty (per"ku-TA'ne-us tranz-LU'min-al KOR'o-nair-e AN'je-o-plas-te) (PTCA). Catheterization is also done on infants and children to examine or treat congenital (kon-JEN'ih-tal) heart defects.
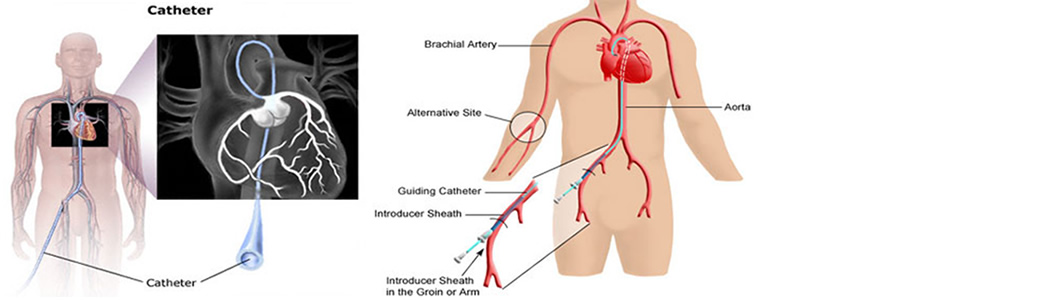
Corornary / Peripheral / Stent Implantation
Stents are small, metal scaffolds similar in size and shape to the spring found in a ballpoint pen. Stent implantation is not appropriate for every artery.
Before stent implantation, the blocked artery usually is treated and dilated with one or more angioplasty balloons. A stent, tightly mounted on a special angioplasty balloon, is then guided to the site of the blockage. The angioplasty balloon is inflated to stretch open the stent and implant it into the walls of the blocked artery. The balloon is deflated and removed, and the stent remains permanently in place to hold the artery open.
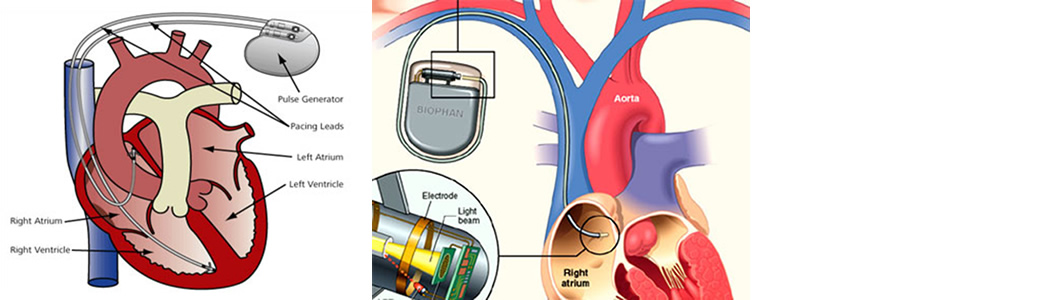
WHAT IS AN AICD?
AICD stand for “automatic implantable cardiac defibrillator”. To explain what an AICD is and what is does, It is explain the problem that it deals with.
As most people know the most common cause of death in the United States has to do with heart disease. Basically, the cause of death is that the heart stops beating and blood circulation ceases. About 1 in 5 people that die do so “suddenly, unexpectedly”.
Over years of research, it has been learned that those people who die “suddenly unexpectedly” do so because their heart develops a condition called ventricular tachycardia which then leads to ventricular fibrillation. These two words describe the condition of a heart that vibrates and quivers but doesn’t have any effective heart beat. It is due to the electrical current that runs the heart, short circuiting and not leading to a rhythmic heart beat as is normal. This electrically chaotic condition develops in hearts that don’t get enough blood or in hearts that are fatigued or in hearts that are sick for various other reasons. But ventricular fibrillation is the final common pathway for the majority of sudden, unexpected deaths.
AICD is implanted usually in the left upper shoulder area. It is connected to the heart through two wires that go through a vein in the upper chest. The AICD has a built in electrocardiogram recorder. It monitors every heart beat and when it sees that a person has developed ventricular fibrillation, it will deliver a shock to convert that rhythm back to normal. The newer devices are so sophisticated that they can often correct an abnormal rhythm before it deteriorates into ventricular fibrillation. When the shock from the AICD occurs, it is definitely an attention getting event. It is physically very disruptive but also the symbolism of what it represents is very frightening.
Unfortunately, an AICD is very, very expensive but fortunately now covered by Medicare for those that have qualifying clinical situations.
Recent research has shown clearly that individuals with an AICD live longer and more comfortable productive lives than those who elect not to use them or those who use medications alone.
Balloon Mitral /Aortic /Pulmonary Valvuloplasty
Heart valve repair is a surgical procedure used to correct a malfunctioning heart valve. Repair usually involves separating the valve leaflets (the one-way "doors" of the heart valve which open and close to pump blood through the heart) or forcing them open with a balloon catheter, a technique known as balloon valvuloplasty.
Coronary Artery Bypass Surgery (CABG)
This is a type of heart surgery. It's sometimes called CABG ("cabbage"). The surgery reroutes, or "bypasses," blood around clogged arteries to improve blood flow and oxygen to the heart.
The arteries that bring blood to the heart muscle (coronary arteries) can become clogged by plaque (a buildup of fat, cholesterol and other substances)This can slow or stop blood flow through the heart's blood vessels, leading to chest pain or a heart attack. Increasing blood flow to the heart muscle can relieve chest pain and reduce the risk of heart attack.
Surgeons take a segment of a healthy blood vessel from another part of the body and make a detour around the blocked part of the coronary artery.
- An artery may be detached from the chest wall and the open end attached to the coronary artery below the blocked area.
- A piece of a long vein in your leg may be taken. One end is sewn onto the large artery leaving your heart -- the aorta. The other end of the vein is attached or "grafted" to the coronary artery below the blocked area.
- Either way, blood can use this new path to flow freely to the heart muscle.
A patient may undergo one, two, three or more bypass grafts, depending on how many coronary arteries are blocked.
Cardiopulmonary bypass with a pump oxygenator (heart-lung machine) is used for most coronary bypass graft operations. This means that besides the surgeon, cardiac anesthesiologist and surgical nurse, a competent perfusionist (blood flow specialist) is required.
During the past several years, more surgeons have started performing off-pump coronary artery bypass surgery (OPCAB). In it, the heart continues beating while the bypass graft is sewn in place. In some patients, OPCAB may reduce intraoperative bleeding (and the need for blood transfusion), renal complications and postoperative neurological deficits (problems after surgery).
Closed Heart Surgery
During closed heart surgery, the surgeon works on structures outside the heart (such as arteries). Sometimes the surgery will completely repair the heart problem; other times it will only fix the heart problem until the child is old enough and strong enough to have the heart defect fixed more completely. Examples of closed heart surgery include repair of coarctation of the aorta, placement of a Pulmonary Artery (PA) Band, Patent Ductus Arteriosus (PDA) ligation, and Blalock-Taussig (BT) shunt. For closed heart surgery, the surgeon will usually make the incision or the opening on the side of the chest, and moves the ribs apart to reach the structures he will repair. This type of surgery does not require the use of cardiopulmonary by-pass.
Open Heart Surgery
Open heart surgery usually involves repairing or fixing structures located inside the heart. With this type of surgery, the incision is usually made in the center of the chest and the breastbone is opened to reach the structures the surgeon will work on. Open heart surgery involves placing the child on a heart-lung bypass machine or cardiopulmonary by-pass. This is also referred to as "a pump" during the operation. Special tubes called cannulae are placed in the arteries and the veins of the heart. Blue blood returning from the body to the heart is sent through the pump where it receives oxygen and then is returned to the body. The child's body temperature is cooled before the child is put on the pump. The child's temperature is lowered so that the cells of the body will need less oxygen and less blood flow during the operation. Some examples of open heart surgeries include fixing a ventricular septal defect (VSD), an atrial septal defect (ASD), the arterial switch operation, the Norwood operation, valve replacements, repair of AV canal, repair of Tetralogy of Fallot, the Fontan operation, and the Ross procedure.
Vascular Surgery
Vascular surgery is the treatment of surgery on diagnosed patients with diseases of the arterial, venous, and lymphatic systems (excluding the intracranial and coronary arteries).
Purpose
Vascular surgery is indicated when a patient has vascular disease that cannot be treated by less invasive, non surgical treatments. The purpose of vascular surgery is to treat vascular diseases, which are diseases of the arteries and veins. Arterial disease is a condition in which blood clots, arteriosclerosis, and other vascular conditions occur in the arteries. Venous disease involves problems that occur in the veins. Some vascular conditions occur only in arteries, others occur only in the veins, and some affect both veins and arteries.
Demographics
As people age, vascular diseases are very common. Since they rarely cause symptoms in the early stages, many people do not realize that they suffer from these diseases. Of the eight million people in the United States who may have peripheral vascular disease (PVD), large percentages are males. In the majority of cases, the blockage is caused by one or more blood clots that travel to the lungs from another part of the body. Factors that increase the chances of vascular disease include:
- increasing age (which results in a loss of elasticity in the veins and their valves)
- a family history of heart or vascular disease
- illness or injury
- pregnancy
- prolonged periods of inactivity sitting, standing, or bed rest
- smoking
- obesity
- hypertension, diabetes, high cholesterol, or other conditions that affect the health of the cardiovascular system
- lack of exercise
Description
Vascular surgery involves techniques relating to endovascular surgeries including: balloon angioplasty and/or stenting, aortic and peripheral vascular endovascular stent/graft placement, thrombolysis, and other adjuncts for vascular reconstruction.
The vascular system is the network of blood vessels that circulate blood to and from the heart and lungs. The circulatory system (made up of the heart, arteries, veins, capillaries, and the circulating blood) provides nourishment to the body's cells and removes their waste. The arteries carry oxygenated blood from the heart to the cells. The veins return the blood from the cells back to the lungs for reoxygenation and recirculation by the heart. The aorta is the largest artery leaving the heart; it then subdivides into smaller arteries going to every part of the body. The arteries, as they narrow, are connected to smaller vessels called capillaries. In these capillaries, oxygen and nutrients are released from the blood into the cells, and cellular wastes are collected for the return trip. The capillaries then connect to veins, which return the blood back to the heart.
The aorta stems from the heart, arches upward, and then continues down through the chest (thorax) and the abdomen. The iliac arteries, which branch out from the aorta, provide blood to the pelvis and legs. The thoracic section of the aorta supplies blood to the upper body, as it continues through the chest. The abdominal section of the aorta, which supplies blood to the lower body, continues through the abdomen.
Vascular diseases are usually caused by conditions that clog or weaken blood vessels, or damage valves that control the flow of blood in and out of the veins, thus robbing them of vital blood nutrients and oxygen. A few common diseases affecting the arteries are peripheral vascular disease (PVD), carotid artery disease, and aortic aneurysms (AAA).
Surgery is used to treat specific diseased arteries, such as atherosclerosis, to help prevent strokes or heart attacks, improve or relieve angina or hypertension, remove aneurysms, improve claudication, and save legs that would otherwise have to be amputated. The choices involve repairing the artery, bypassing it, or replacing it.
As people age, atherosclerosis, commonly called hardening of the arteries, occurs with the constant passage of blood through the arteries. It can take on a number of forms, of which atherosclerosis (hardening of the innermost portion) is the most common. This occurs when fatty material containing cholesterol or calcium (plaque) is deposited on the innermost layer of the artery. This causes a narrowing of the inside diameter of the blood vessel. Eventually, the artery becomes so narrow that a blood clot (thrombus) forms, and blocks blood flow to an entire portion of the body. This condition is called PVD or peripheral arterial disease. In another form of atherosclerosis, a rough area or ulcer forms in the diseased interior of the artery. Blood clots then tend to develop on this ulcer, break off, and travel further along, forming a blockage where the arteries get narrower. A blockage resulting from a clot formed elsewhere in the body is called an embolism.
People who have few areas affected by PVD may be treated with angioplasty by opening up the blood vessel with a balloon placed on the end of a catheter. A stent is often used with angioplasty to help keep the artery open. The type of surgery used to treat PVD is based upon the size and location of the damaged artery. The following are surgery techniques used for severe PVD:
- Bypass surgery is preferred for people who have many areas of blockage or a long, continuous blockage.
- Aortobifemoral bypass is used for PVD affecting the major abdominal artery (aorta) and the large arteries that branch off of it.
- In a technique called thromboendarterectomy, the inner diseased layers of the artery are removed, leaving the relatively normal outer coats of the artery.
- Resection involves a technique to remove a diseased artery following an aneurysm; a bypass is created with a synthetic graft.
- In a bypass graft, a vein graft from another part of the body or a graft made from artificial material is used to create a detour around a blocked artery.
- Tibioperoneal bypass is used for PVD affecting the arteries in the lower leg or foot.
- Femoro Popliteal (fem-pop) bypass surgery is used for PVD affecting the arteries above and below the knee.
- Embolectomy is a technique in which an embolic clot on the wall of the artery is removed, using an inflatable balloon catheter.
- Thrombectomy is a technique in which a balloon catheter is inserted into the affected artery beyond a blood clot. The balloon is then inflated and pulled back, bringing the clot with it.
An aneurysm occurs when weakened blood vessels bulge like balloons as blood flows through them. Once they have grown to a certain size, there is a risk of rupture and life-threatening bleeding. There are two types of aortic aneurysms: abdominal aortic aneurysm (AAA) and thoracic aortic aneurysm. This classification is based on where the aneurysm occurs along the aorta. Aneurysms are more common in the abdominal section of the aorta than the thoracic section.
Most blood clots originate in the legs, but they can also form in the veins of arms, the right side of the heart, or even at the tip of a catheter placed in a vein. The following venous disease conditions usually occur in the veins of the legs:
- varicose veins
- phlebitis
- venous stasis disease
- deep vein thrombosis (DVT)
- claudication
- blood clots
Carotid artery disease is a condition in which the arteries in the neck that supply blood to the brain become clogged; this condition can cause a stroke.
Lymphatic obstruction involves blockage of the lymph vessels, which drain fluid from tissues throughout the body and allow immune cells to travel where they are needed. Some of the causes of lymphatic obstruction(also known as swelling of the lymph passages), include infections such as chronic cellulitis, or parasitic infections such as filariasis, trauma, tumors, certain surgeries including mastectomy, and radiation therapy. There are rare forms of congenital lymphedema that probably result from abnormalities in the development of the lymphatic vessels. Most patients with lymphedema will not need surgery, as the symptoms are usually managed by other techniques. Surgical therapy for lymphedema includes removal of tissue containing abnormal lymphatics, and less commonly, transplant of tissue from areas with normal lymphatic tissues to areas with abnormal lymphatic drainage. In rare cases, bypass of abnormal lymphatic tissue is attempted, sometimes using vein grafts.
Other examples of vascular surgery include:
- cerebral aneurysm
- acute arterial and graft occlusion
- carotid Endarterectomy
- endovascular grafting
- Vasculogenic erectile dysfunction
- renal artery aneurysm
- surgery on varicose veins
- lower extremity amputation
Diagnosis/Preparation
In order for a patient to be diagnosed with a vascular disease, they must be clinically evaluated by a vascular surgeon, which includes a history and physical examination. A vascular surgeon also treats vascular disorders by non-operative means, including drug therapy and risk factor management.
The symptoms produced by atherosclerosis, thrombosis, embolisms, or aneurysms depend on the particular artery affected. These conditions can sometimes cause pain, but often there are no symptoms at all.
A physician has many ways of feeling, hearing, measuring, and even seeing arterial blockages. Many arteries in the body can be felt or palpated. A doctor can feel for a pulse in an area he or she believes afflicted. Usually the more advanced the arteriosclerosis, the less pulse in a given area.
As the artery becomes blocked, it can cause a noise very much like water roaring over rocky rapids. Your physician can listen to this noise (bruit) directly, or can use special amplification systems to hear the noise.
There are other tests that can be done to determine if arterial blood flow is normal:
- ankle-brachial index (ABI) test
- arteriogram
- segmental pressure test
- ultrasound scan
- magnetic resonance imaging
- computed tomography scan
- angiography
- lymphangiography
- lymphoscintigraphy
- plethysmography
- duplex ultrasound scanning
There may be no symptoms of vascular disease caused by blood clots until the clot grows large enough to block the flow of blood through the vein. The following symptoms may then come on suddenly:
- pain
- sudden swelling in the affected limb
- reddish blue discoloration
- enlargement of the superficial veins
- skin that is warm to the touch
The physician will probably do an evaluation of all organ systems including the heart, lungs, circulatory system, kidneys, and the gastrointestinal system. The decision whether to have surgery or not is based on the outcome of these evaluations.
For high-risk patients undergoing vascular surgery, research has shown that taking oral beta-blockers one to two weeks before surgery and continuing for at least two weeks after the operation can significantly reduce the chance of dying or having a heart attack. Scientists suspect that the drug improves oxygen balance in the wall of the heart and stabilizes plaques in the arteries.
Aftercare
The length of time in intensive care and hospitalization will vary with each surgery, as will the recovery time, depending on numerous factors. Because surgery for an AAA is more serious, the patient can expect to be in intensive care for 24 hours, and in the hospital for five to 10 days, providing the patient was healthy and had a smooth operative and postoperative course. If there are complications, the hospital stay will likely increase. It may take as long as six months to fully recover from surgery for an AAA.
Living a "heart-healthy lifestyle" is the best way of preventing and controlling vascular disease: do not smoke; eat nutritious foods low in fat; exercise; maintain a healthy weight; and control risk factors such as high blood pressure, high cholesterol, diabetes, hypertension, and other factors that contribute to vascular disease.
Medications that may be used to treat PVD include:
- aspirin and other antiplatelet medications to treat leg pain
- statins to lower cholesterol levels
- medications to control high blood pressure
- medications to control diabetes
- anticoagulants are rarely, but not generally, used to treat PVD unless the person is at an increased risk for forming blood clots
Risks
All surgeries carry some risks. There is a risk of infection whenever incisions are required. Operations in the chest or those that involve major blood vessels carry a higher risk of complications. Patients who smoke, have high blood pressure, chronic lung or kidney disease, or other illnesses are at greater risk of complications during and after surgery. Other risks of vascular surgery include:
- bleeding
- failed or blocked grafts
- heart attack or stroke
- leg swelling if a leg vein is used
- people over 65 years are at greater risk for brain impairment after major surgery
- the more damaged the circulatory system is before surgery, the higher susceptibility to mental decline after vascular surgery
- impotence
The patient should discuss risks with their surgeon after careful review of the patient's medical history and a physical examination.
Normal Results
The success rate for vascular surgery varies depending on a number of factors which may influence the decision on whether to have surgery or not, as well as the results.
The chance that an aneurysm will rupture generally increases with the size of the aneurysm; AAAs smaller than 1.6 in (4 cm) in diameter have up to a 2% risk of rupture while ones larger than 2 in (5 cm) in diameter have a 22% risk of rupture within two years.
Arterial bypass surgery and peripheral bypass surgery have very good success rates. Most of those who undergo AAA surgery recover well, except in the case of a rupture. Most patients who have a ruptured aortic aneurysm die. Surgery for an already ruptured aneurysm is not usually successful, due to excessive, rapid blood loss.
Surgical therapy for lymphedema has met with limited success, and requires significant experience and technical expertise.
Morbidity and Mortality Rates
Peripheral vascular disease affects 10 million people in the United States, including 5% of those over 50. Only a quarter of PVD sufferers are receiving treatment. More than five million people in the United States develop DVT each year. More than 600,000 Americans experience a pulmonary embolism every year. Of those, approximately 200,000 people die from the condition.
Alternatives
There a few alternatives to treating vascular disease, although extensive research has not been done. Acupuncture is used to aid in hypertension and chelation therapy is thought to stabilize the effects of vascular disease. The focus should be on maintaining a proper diet and being aware of a family history of vascular disease so as to catch it as early as possible.
Thoracic Surgery
Thoracic surgery is any surgery performed in the chest (thorax).
Purpose
The purpose of thoracic surgery is to treat diseased or injured organs in the thorax, including the esophagus (muscular tube that passes food to the stomach), trachea (windpipe that branches to form the right bronchus and the left bronchus), pleura (membranes that cover and protect the lung), mediastinum (area separating the left and right lungs), chest wall, diaphragm, heart, and lungs. General thoracic surgery is a field that specializes in diseases of the lungs and esophagus. The field also encompasses accidents and injuries to the chest, lung cancer, lung transplantation, and surgery for emphysema.
Description
The most common diseases requiring thoracic surgery include lung cancer, chest trauma, emphysema, and lung transplantation.
Lung Cancer
Lung cancer is one of the most significant public health problems in the United States and the world. Approximately 171,600 new cases of lung cancer occurred in 1999. It accounts for 28% of cancer deaths, 14% of all cancer diagnoses, and is the leading cause of cancer deaths among women and second most common cause of male cancer deaths. The five-year survival rate in localized disease can approach 50% (stages I and II).
Lung cancer develops primarily by exposure to toxic chemicals. Cigarette smoking is the most important risk factor responsible for the disease. Other environmental factors that may predispose a person to lung cancer include such industrial substances as arsenic, nickel, chromium, asbestos, radon, organic chemicals, air pollution, and radiation.
Most cases of lung cancer develop in the right lung because it contains the majority (55%) of lung tissue. Additionally, lung cancer occurs more frequently in the upper lobes of the lung than in the lower lobes. The tumor receives blood from the bronchial artery (a major artery in the pulmonary system).
Adenocarcinoma of the lung is the most frequent type of lung cancer, accounting for 45% of all cases. This type of cancer can spread (metastasize) earlier than another type of lung cancer called squamous cell carcinoma (which occurs in approximately 30% of lung cancer patients). Approximately 66% of squamous cell carcinoma cases are centrally located. They expand against the bronchus, causing compression. Small-cell carcinoma accounts for 20% of all lung cancers; and the majority (80%) are centrally located. Small-cell carcinoma is a highly aggressive lung cancer, with early metastasis to such distant sites as the brain and bone marrow (the central portion of certain bones, which produce formed elements that are part of blood).
Most lung tumors are not treated with thoracic surgery since patients seek medical care later in the disease process. Chemotherapy increases the rate of survival in patients with limited (not advanced) disease. Surgery may be useful for staging or diagnosis. Pulmonary resection (removal of the tumor and neighboring lymph nodes) can be curative if the tumor is less than or equal to 3 cm, and presents as a solitary nodule. Lung tumors spread to other areas through neighboring lymphatic channels. Even if thoracic surgery is performed, postoperative chemotherapy may also be indicated to provide comprehensive treatment (i.e., to kill any tumor cells that may have spread via the lymphatic system).
Genetic engineering has provided insights related to the growth of tumors. A genetic mutation called a k-ras mutation frequently occurs, and is implicated in 90% of genetic mutations for Adenocarcinoma of the lung. Mutations in the cancer cells make them resistant to chemotherapy, necessitating the use of multiple chemotherapeutic agents.
Chest Trauma
Chest trauma is a medical/surgical emergency. Initially, the chest should be examined after an airway is maintained. The mortality (death) rate for trauma patients with respiratory distress is approximately 50%. This figure rises to 75% if symptoms include both respiratory distress and shock. Patients with respiratory distress require endotracheal intubation (passing a plastic tube from the mouth to the windpipe) and mechanically assisted ventilator support. Invasive thoracic procedures are necessary in emergency situations.
Trauma requiring urgent thoracic surgery may include any of the following problems: a large clotted hemothorax, massive air leak, esophageal injury, valvular cardiac (heart) injury, proven damage to blood vessels in the heart, or chest wall defect.
Emphysema
Lung volume reduction surgery (LVRS) is the term used to desribe surgery for patients with emphysema. LVRS is intended to help persons whose disabling dyspnea (difficulty breathing) is related to emphysema and does not respond to medical management. Breathlessness is a result of the structural and functional pulmonary and thoracic abnormalities associated with emphysema. Surgery will assist the patient, but the primary pathogenic process that caused the emphysema is permanent because lung tissues lose the capability of elastic recoil during normal breathing (inspiration and expiration).
Patients are usually transferred out of the intensive care unit within one day of surgery. Physical therapy and rehabilitation (coughing and breathing exercises) begin soon after surgery, and the patient is discharged when deemed clinically stable.
Diagnosis/Preparation
The surgeon may use two common incisional approaches: sternotomy (incision through and down the breastbone) or via the side of the chest (thoracotomy).
An operative procedure known as video assisted thoracoscopic surgery (VATS) is minimally invasive. During VATS, a lung is collapsed and the thoracoscopic and surgical instruments are inserted into the thorax through any of three to four small incisions in the chest wall.
Another approach involves the use of a mediastinoscope or bronchoscope to visualize the internal anatomical structures during thoracic surgery or diagnostic procedures.
Preoperative evaluation for most patients (except emergency cases) must include cardiac tests, blood chemistry analysis, and physical examination. Like most operative procedures, the patient should not eat or drink food 10–12 hours prior to surgery. Patients who undergo thoracic surgery with the video-assisted approach tend to have shorter inpatient hospital stays.
Aftercare
Patients typically experience severe pain after surgery, and are given appropriate medications. In uncomplicated cases, chest and urine (Foley catheter) tubes are usually removed within 24–48 hours. A highly trained and comprehensive team of respiratory therapists and nurses is vital for postoperative care that results in improved lung function via deep breathing and coughing exercises.
Risks
Precautions for thoracic surgery include coagulation blood disorders (disorders that prevent normal blood clotting) and previous thoracic surgery. Risks include hemorrhage, myocardial infarction (heart attack), stroke, nerve injury, embolism (blood clot or air bubble that obstructs an artery), and infection. Total lung collapse can occur from fluid or air accumulation, as a result of chest tubes that are routinely placed after surgery for drainage.
Diabetes
Diabetes is a condition in which the amount of glucose in the blood is too high. This happens when the body's method of converting glucose into energy does not work properly and allows the level of glucose to rise. The process that converts glucose into energy relies on a hormone known as insulin. When the supply of insulin stops or it becomes ineffective, blood glucose levels can rise and result in diabetes.
Type I Diabetes
Type I diabetes is also known as Insulin Dependent. It develops if the body is not able to produce insulin. Type I diabetes usually occurs in people under the age of 40, often in early childhood
Type II Diabetes
Type II diabetes is also known as Non-Insulin Dependent Diabetes. It develops when the body produces some but not enough of the insulin it needs, or when the body is not able to use the insulin properly It is often found in people who are overweight.
The diet can be planned individually by a Dietitian / Nutritionist to suit the person's lifestyle
Myths
The dietary advice for people with diabetes has changed considerably- over the last century. At one point people with diabetes were told to starve themselves!
Some years later people with diabetes were told to eliminate all sugar and sugary foods from their diet.
Facts
Today, however, the most important message for people with diabetes is to eat healthy food, in exactly the same way that is recommended for the whole population - that is a balanced diet based on fiber rich cereals, pulses and plenty of vegetables, and is low in fat, salt and sugar. So the good news is that a small amount of refined cereals like refined flour (maida), semolina, vermicilli, white bread; root vegetables like potatoes, yam, sweet potato, colocasia; sugar and sugar-containing foods can be eaten, preferably as pert of a healthy meal.
We need energy to live but the balance between carbohydrate, fat and protein must be right for us to remain healthy.
- Too little protein can interfere with growth and other body functions.
- Too much fat can lead to obesity and is a risk factor in heart diseases.
The Balance of Good Health should be based on the 'Nine Guidelines for a Healthy Diet', which are:
- Enjoy your food
- Eat a variety of different foods
- Eat the right amount to be a healthy weight
- Eat plenty of foods rich in complex carbohydrate and fiber
- Eat plenty of fruit and vegetables
- Take small frequent meals
- Don't eat too many foods that contain lot of fat
- Don't have sugary foods like jams, jellies and jaggery too often
If you drink alcohol, drink within sensible limits
Eat plenty of foods rich in Complex Carbohydrates and Fiber
Eating more complex carbohydrate rich foods leads to gradual increase in blood sugar levels. This helps in better control of diabetes. Some rich sources of complex carbohydrates are:-
- Whole grain like oatmeal, unpolished rice, ragi, barley- and bajra roti;
- Whole wheat flour mixed with soy flour chapatti, adai, pesarattu, brown bread, etc.
Benefits of Fiber
Foods high in soluble fiber like cluster beans, guava, kidney beans (rajmah), gum acacia helps:
- Delay absorption of carbohydrates and hence are unlikely to cause sudden rise in blood glucose levels;
- Prevent constipation and reduce blood cholesterol and triglyceride levels thus helping to prevent heart disease.
Intake of Protein rich foods is a must
Proteins are essential for growth, development and tissue repair. There might be increased loss of protein in diabetic patients hence it is essential to consume slightly higher protein than required by a normal person.
Some rich sources of protein are:-
- Fish, chicken, egg whites;
- Skimmed milk and milk based preparations;
- Pulses, soybean and nuts*.
However, people with kidney disease (nephropathy) should restrict their protein intake. They need to consult their doctor/nutritionist to know the exact protein allowance.
Don't eat too many foods that contain a lot of fat
High level of fats or lipids in your blood can cause heart disease, heart attack and stroke. It is therefore very important that you keep your lipids at a healthy level.
- Use 3 tsp of oil in your food on a daily basis or half a liter /month.
- Choose leaner cuts of meat and lower fat version of foods such as skimmed or semi-skimmed milk or low-fat curd and cheese.
- Trim all visible fat and skin from meat and poultry and choose cooking methods that do not add fat, for example grill/bake/roast instead of fry.
Eat five portions of Fruits and Vegetables daily.
Some people are not sure whether they can take fruits or not. However, there is no reason to avoid all naturally occurring fructose in fruits, vegetables, and other foods.
- Fruits and vegetables are low in fat and high in fiber, so help to achieve the right balance between the nutrients in the diet.
- They also contain vitamins, minerals and other substances known as phytochemicals which together help protect us from diseases such as cancer and heart disease. Moreover, liberal intake of B-Vitamins have shown to help prevent nerve damage in diabetics.
Fruit juices on the other hand contain a lot of sugar because plenty of fruits go into making a glass of juice hence they should be avoided. In addition, fruit juices do not add fiber as most of it is strained which in turn can raise blood sugar level instantaneously.
* Nuts are rich sources of monounsaturated fatty acids. These are helpful in improving lipid profiles (Cholesterol Levels).
Good Health Tips
Plan the type of foods eaten during meals
Combining protein, fat, and carbohydrates during meals and snacks e.g., . eating mixed vegetable and sprouted dal upma/ pulao; . chapatti with vegetables/chicken/fish; can lead to better control of blood glucose levels and less insulin release than consuming meals or snacks that consist primarily of carbohydrates and fats e.g., . potato finger chips, potato bonda, puri with potato bhaji etc.
Take small frequent meals
- Eating large meals at one time should be avoided.
- Never skip or delay your meals.
- Fasting and crash dieting methods can be dangerous for diabetics.
- Your meal plan should include 3 main meals and 2-3 snacks per day for e.g., bhelpuri, vegetable poha, dhokla, marie biscuits, fruits, nuts (6-7), roasted bengal gram along with nutritional beverage specially designed for diabetics. This reduces the chances of sudden high or low peaks in blood sugar levels.
Healthy weight
One of the most important keys to the successful management of diabetes is to remain within your ideal weight range. The Body Mass Index, or BMI is a simple calculation that has been developed as a guide for adults to achieve a healthy weight for their height. There is no one perfect weight, rather a weight range, which allows for differences in people's build and frame size.
Healthy Shape
Excess fat carried around the waist has been shown to be a greater risk factor for diseases such as heart disease and diabetes than carrying excess fat around the hips, thighs and buttocks.
Men are genetically predisposed to carry excess weight around their abdomen giving them an apple shape, whereas women are more likely to be pear-shaped as excess weight is carried around the hips.
Limits in terms of increased risk and substantial risk for the waist measurements of men and women.
Unfortunately, there is nothing you can do to influence which areas you can gain or lose might from. There are no diets or eating plans that will enable you to spot reduce (for example, only lose weight from your tummy while maintaining your curves).
Exercise can help tone up specific muscle groups and of course will help burn fat.
Exercise :
1. Benefits for Diabetics
- It works together with insulin to lower the level of blood sugar
- Helps to lower blood lipid levels
- Improves circulation and hence help to reduce blood pressure
- Helps to reduce weight
- In addition keeps you fit and makes you feel good
2. Points to remember
- Don't exercise on an empty stomach as it may cause low blood sugar or hypoglycemia
- Always keep candies or sugar cubes with you while exercising so that you can pop them up if you experience signs of low blood sugar levels in your body
- Exercise should be done regularly and preferably at the same time of the day
- Warm up well before exercise
3. Caution! Stop exercise and seek immediate medical care if you have any of the following:
- Tightness in your chest
- Severe shortness of breath
- Chest pain or pain in your arm, jaw, often on the left side
- Palpitation
- Dizziness
- Feeling of faintness